
Figure 16.2.1 One Nephron of the Kidney
return to the Course index
previous | next
There are three major renal excretion processes to consider; 1) glomerular filtration; 2) tubular secretion; and 3) tubular re-absorption

Figure 16.2.1 One Nephron of the Kidney
Again, most drugs are filtered from blood in the glomerular, the overall renal excretion however is controlled by what happens in the tubules. More than 90% of the filtrate is reabsorbed. 120 ml/min is 173 L/day. Normal urine output as you may realize is much less than this, about 1 to 2 liter per day.
Drugs or compounds which are extensively secreted, such as p-aminohippuric acid (PAH), may have clearance values approaching the renal plasma flow rate of 425 to 650 ml/min, and are used clinically to measure this physiological parameter (see Documenta Geigy).
Many drugs are either weak bases or acids and therefore the pH of the filtrate can greatly influence the extent of tubular re-absorption for many drugs. When urine is acidic weak acid drugs tend to be reabsorbed. Alternatively when urine is more alkaline, weak bases are more extensively reabsorbed. Making the urine more acidic can cause less reabsorption of weak bases or enhanced excretion. These changes can be quite significant as urine pH can vary from 4.5 to 8.0 depending on the diet (e.g. meat can cause a more acidic urine) or drugs (which can increase or decrease urine pH).
In the case of a drug overdose it is possible to increase the excretion of some drugs by suitable adjustment of urine pH. For example, in the case of pentobarbital (a weak acid) overdose it may be possible to increase drug excretion by making the urine more alkaline with sodium bicarbonate injection.
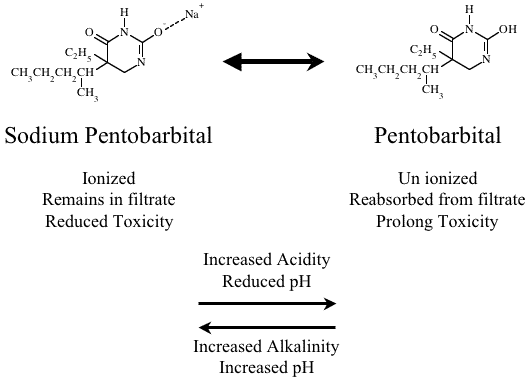
Figure 16.2.2 Pentobarbital Ionization
This method is quite effective if the drug is extensively excreted as the unchanged drug (i.e. fe approaches 1). If the drug is extensively metabolized then alteration of kidney excretion will not alter the overall drug metabolism all that much.
The effect of pH change on tubular re-absorption can be predicted by consideration of drug pKa according to the Henderson-Hesselbalch equation.

Equation 16.2.1 Rate of Excretion
Remember that renal clearance can be calculated as part of the total body clearance for a particular drug. Renal clearance can be used to investigate the mechanism of drug excretion. If the drug is filtered but not secreted or reabsorbed the renal clearance will be about 120 ml/min in normal subjects. If the renal clearance is less than 120 ml/min then we can assume that at least two processes are in operation, glomerular filtration and tubular re-absorption. If the renal clearance is greater than 120 ml/min then tubular secretion must be contributing to the elimination process. It is also possible that all three processes are occurring simultaneously. The drug renal clearance value can be compared with physiologically significant values, e.g. glomerular filtration rate (GFR) of approximately 120 ml/min or renal plasma flow of about 650 ml/min.
Renal clearance is then:

Equation 16.2.2 Renal Clearance

Equation 16.2.3 Renal clearance expanded (Bauer, p 14)
The influence of fU, GFR, (CLisec and fR can be explored using the interactive graph to calculate plasma concentrations after iv bolus or oral dosing.
Renal clearance values can range from 0 ml/min, the normal value for glucose which is usually completely reabsorbed to a value equal to the renal plasma flow of about 650 ml/min for compounds like p-aminohippuric acid.
We can calculate renal clearance using the pharmacokinetic parameters ke and V. Thus CLrenal = ke • V. Renal clearance can also be determined as U∞/AUC. We can calculate renal clearance by measuring the total amount of drug excreted over some time interval and dividing by the plasma concentration measured at the midpoint of the time interval. (This was part of a laboratory experiments -- first beaker experiment).

Equation 16.2.4 Renal Clearance

Equation 16.2.5 Renal Clearance
To continue we can briefly look at some other routes of drug excretion. We will then return to the topic of renal excretion by considering drug dosage adjustments in patients with reduced renal function.
Material on this website should be used for Educational or Self-Study Purposes Only
Copyright © 2001 - 2026 David W. A. Bourne (david@boomer.org)
 | Pharmacy Math Part One A selection of Pharmacy Math Problems |
 |